Laparoscopic Surgery
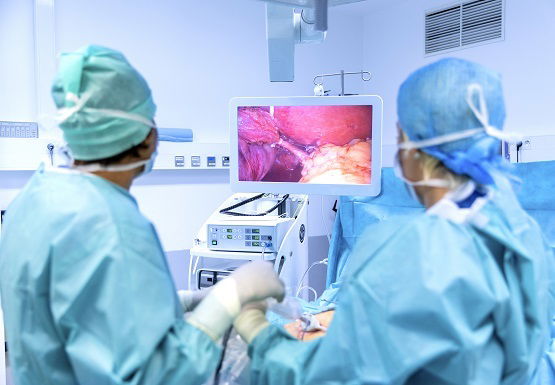
Laparoscopic Surgery
Laparoscopy - Gynecologic
Introduction
A laparoscopy is a minimally invasive surgical procedure that uses a laparoscope to view the internal female reproductive organs. A laparoscope is a type of endoscope. It consists of a thin tube with a light and viewing instrument. Images from the laparoscope may be sent to a video monitor. A laparoscopy may be used to identify abnormalities and diagnose disease. It may also be used during complex operations.
Historically, exploratory laparoscopy was used to diagnose ovarian disease, cysts, endometriosis, fibroids, and cancer. Its use has expanded to include removal of tubal pregnancies, harvesting eggs for in vitro fertilization, and removal of the uterus (hysterectomy) or ovaries (oophorectomy).
Treatment
A laparoscopy is usually performed at a surgical center or hospital. It may be an outpatient procedure or involve a short inpatient stay, depending on the case. General anesthesia is used, and you will need to have someone else drive you home after your surgery.
You will be advised not to eat or drink for typically eight hours before your procedure. You will wear an examination gown and lie on your back on an examination table for the procedure. After you are anesthetized, a catheter will be gently inserted through your urethra and into your bladder to collect urine during your surgery. Your surgical area will be carefully cleaned.
Your doctor will make a small incision near your belly button. Carbon dioxide air will be administered through the incision to raise the abdominal wall and create a space for your surgeon to view your organs and work in. Additional small incisions will be made to insert the laparoscope.
After your examination or procedure, the incisions are closed with a few stitches and covered with bandages. The catheter is carefully removed. You will be taken to a recovery area where you will be observed until you wake up.
Following your procedure, your incision sites may throb or feel slightly painful. Your doctor will recommend or prescribe a pain reliever for you. You may feel an increase urge to urinate because the carbon dioxide may temporarily put pressure on your bladder. You may experience temporary irritation when you urinate because of the catheter. Your doctor will provide you with a written list of precautions, wound care directions, and temporary restrictions.
Your doctor may let you know the results of your examination, but may wait to thoroughly review the results of your laparoscopy during a follow-up appointment or phone call, when you are more alert. Your incision sites will be examined at your follow-up appointment. Your stitches will be removed.
Laparoscopic surgery is a minimally invasive, video-guided technique that has revolutionized the field of surgery. Instead of making a large incision through the skin and underlying muscles (laparotomy), a laparoscopic surgeon makes just a few tiny incisions, one for a long, narrow telescope with a camera attached, and two or three others for the instruments needed. In pelvic laparoscopic surgery, the entry port for the camera is generally through the navel. The entry ports for the instruments are generally just half-inch or smaller incisions in the groin area.
The procedure begins with the introduction of a gas, usually carbon dioxide, into the pelvic cavity to provide adequate working space. Then the camera is inserted so that the surgeon can clearly see a magnified view of the pelvic organs. Specially designed instruments enable the surgeon to perform all the delicate maneuvers needed to remove diseased tissue, introduce needed materials (such as mesh in cases of pelvic floor repair) and suture.
Because there is less trauma to the body, recovery is much faster than with traditional, open abdominal surgery, and there is less pain. Patients can often get up and move around within a few hours of surgery. Hospital stay is reduced to a day, if needed at all. Many procedures can be done on an outpatient basis.
Another advantage is reduced risk of infection, because tissues are not exposed as they are in open surgery.
Because it requires sophisticated equipment, laparoscopic surgery is expensive, and not all hospitals are able to offer it. It also requires specialized training, even for surgeons who are experts at open surgery. They must learn to transfer their skills at working in a three-dimensional situation to working from a two-dimensional video screen. However, as more and more young surgeons who have grown up in the computer age enter the field, the supply of qualified laparoscopic surgeons will multiply.
Questions to ask your doctor
If you need surgery for a pelvic disorder, it is appropriate to ask your doctor everything you need to know. Most doctors welcome the chance to explain things to you, because an informed patient is a better patient. Most doctors also welcome a second opinion to confirm their own conclusions. Never be afraid to ask questions.
- What is causing my problem?
- Do we need to confirm this diagnosis with other tests? What are their side effects, risks and costs?
- What treatment do you recommend?
- Can my condition be treated with a minimally invasive surgical technique?
- What is the risk if we “wait and see?”
- Can you do this procedure, or do I need a specialist?
- How many patients have you treated for a condition just like mine?
- What are the success rates of this procedure?
- What are the possible complications, and how often do they occur?
- What will be involved in my recovery?
- What is the impact of this surgery on my ability to have children?
- Will this treatment affect my sexual function?
- What is the risk of recurrence of my condition?
- Should I get a second opinion?
References
- American Society for Reproductive Medicine. Laparoscopy and hysteroscopy: A guide for patients. Patient Information Series 2006. www.asrm.org/Patients/patientbooklets/ laparoscopy.pdf
- eMedicineHealth. Laparoscopy. www.emedicinehealth.com/laparoscopy/article_em.htm
- Medina M. About laparoscopy and endoscopy: Laparoscopic surgery. Society of Laparoendoscopic Surgeons. 2004. http://www.sls.org/ | http://www.laparoscopy.org