Polycystic Ovarian Syndrome (PCOS)
Introduction
Polycystic ovary disease is a common type of hormone disorder. It causes enlarged ovaries that contain numerous cysts. Polycystic ovary disease may also lead to infertility, excess hair growth, and heavy, irregular, or absent periods. Treatments include medications and weight reduction.
Anatomy
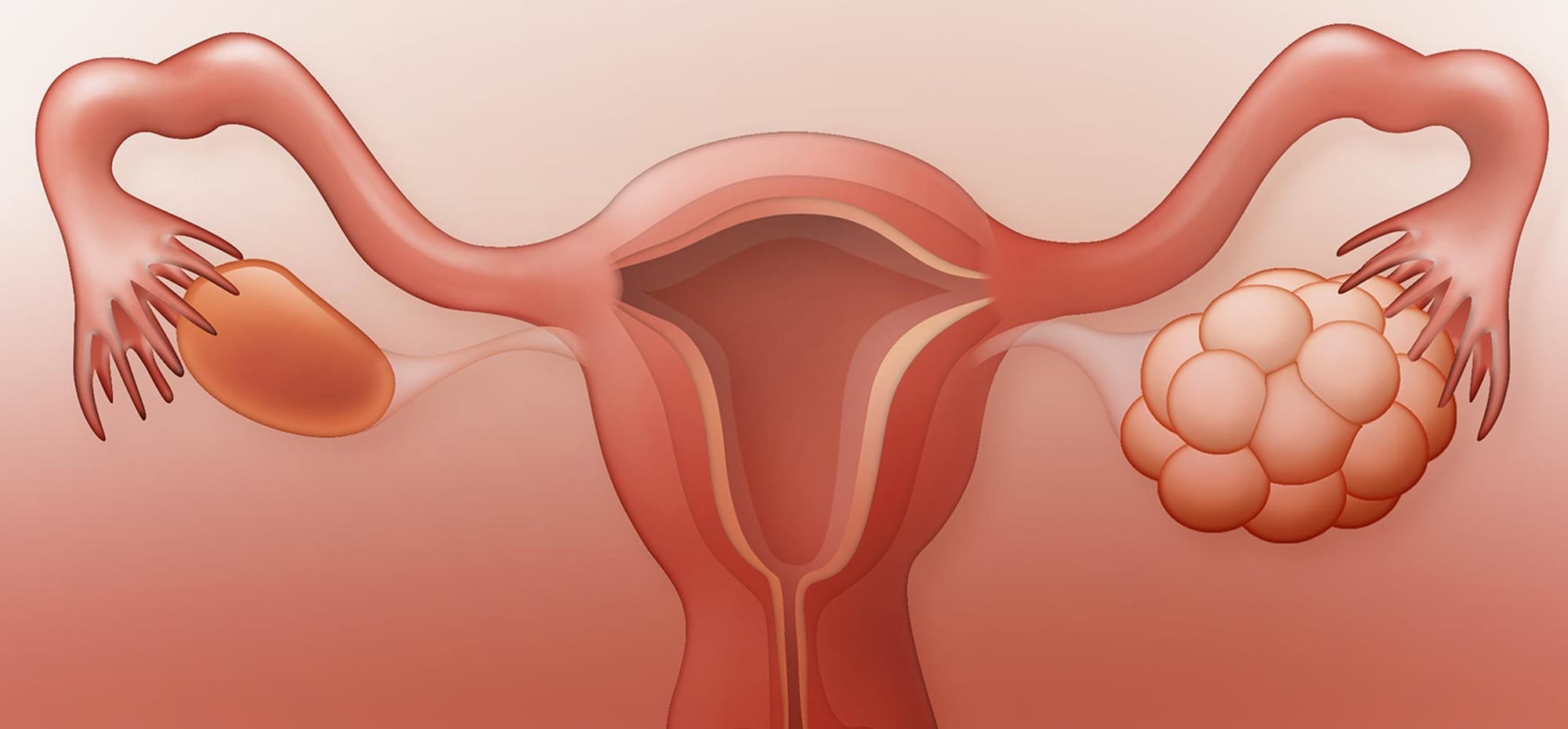
The ovaries are two small organs that produce eggs and hormones. The ovaries contain follicles that produce and release an egg into the fallopian tubes each month. Hormones, including lutenizing hormone (LH) and follicle-stimulating hormone (FSH), regulate your menstrual cycle. These hormones are produced by the pituitary gland in your brain.
Causes
The exact cause of polycystic ovary disease is unknown. Polycystic ovary disease results when a problem occurs with the normal hormone cycle. Low levels of FSH and high levels of androgens (male hormones) do not allow egg follicles in the ovaries to develop and release eggs. Instead, the follicles form multiple small cysts within the ovary. High levels of insulin in the blood can also interfere with ovulation and contribute to polycystic ovary disease.
Polycystic ovaries are two to five times larger than healthy ovaries. They have a thick white covering and are filled with a high number of follicles are various stages of development. Polycystic ovary disease is most frequently diagnosed in women during their twenties or thirties. Women with polycystic ovary disease may need fertility treatments to make pregnancy possible.
Symptoms
Polycystic ovary disease can produce a variety of symptoms. Your periods may change and become irregular, heavy, very light, or absent. You may experience infertility. You may gain weight or become obese. Unwanted hair may grow on your face or body. You may develop male sex characteristics, such as a deepening voice, male pattern baldness, or decreased breast size. Acne may become worse. You may be diagnosed as having insulin resistance or diabetes.
Diagnosis
You should meet with your doctor if your menstrual pattern changes or if you experience excessive weight gain, facial hair growth, or acne. You should tell your doctor about your symptoms. Your doctor will review your medical history. Blood tests may be used to test your hormone and insulin levels. Your blood and urine may be tested for signs of diabetes. Your doctor will conduct a physical examination, including a pelvic examination. In some cases, imaging tests may be used.
An ultrasound may be used to show the size of your ovaries and the thickness of their coverings. Ultrasound testing is painless. Your doctor or a radiation technologist will gently place and move a conduction device on your skin. The conduction device transmits sound waves to a computer that creates images on a video monitor. A transvaginal ultrasound may be used to obtain even more detailed pictures. For a transvaginal ultrasound, a conduction wand is gently inserted into your vagina during the test.
Treatment
Treatment for polycystic ovarian disease may involve hormone medications or medications to help your body use insulin better. Reducing your weight can be very helpful for lowering insulin levels. Ask your doctor for referrals or recommendations to help with weight loss. Your doctor can recommend other treatments for symptoms that bother you, such as acne or unwanted hair growth. A fertility specialist may use hormone medications or surgical procedures to help increase your chances of becoming pregnant. Your blood pressure, cholesterol, weight, blood sugar, and insulin levels will be regularly monitored and treated to help prevent heart disease and complications from diabetes.
Prevention
If you have polycystic ovary disease, it is important to reduce the risk factors that are controllable to benefit your health and prevent future problems. Ask your doctor about ways to reduce your weight safely, eat healthy, and exercise. Regulating and monitoring your blood pressure, weight, blood sugar, and insulin may help prevent diabetes and heart-related complications.
Am I at Risk
Risk factors may increase your likelihood of developing polycystic ovary disease, although some people that develop the condition do not have any risk factors. People with all of the risk factors may never develop the disease; however, the chance of developing polycystic ovary disease increases with the more risk factors you have. You should tell your doctor about your risk factors and discuss your concerns.
Risk factors for polycystic ovary disease:
_____ Insulin resistance or high blood insulin levels are associated with polycystic ovary disease.
_____ Obesity increases the risk of polycystic ovary disease. Women that carry body fat on their abdomen tend to have a higher risk than women with body fat that is distributed throughout their body.
_____ Researchers think that genetics may play a role in polycystic ovary disease. If your mother or sisters have polycystic ovary disease, your risk is increased.
Complications
Infertility can be a complication of polycystic ovary disease. Pregnancy may be achieved with fertility treatments. Women with polycystic ovary disease have an increased risk for breast cancer and endometrial cancer. An increase in male hormones may cause hair growth and acne, conditions that your doctor may help to resolve.
Polycystic ovary syndrome or PCOS is a common reproductive hormonal disorder that prevents ovulation and leads to an increased accumulation of male hormones. The ovaries become filled with small cysts, further blocking ovulation. Because of the increase in male hormones, a woman may experience excess hair growth, oily skin, acne and infertility, in addition to irregular, heavy periods. PCOS affects about 5% of women. Additionally constant estrogen production unaccompanied by progesterone may lead to hyperplasia of the uterine lining cells, which in turn may develop into the precancerous condition known as atypical hyperplasia over a period of years. Some women with PCOS may also be predisposed to diabetes.
Treatment Options
PCOS is successfully treated with the female hormone progesterone, which is normally produced after ovulation and produces menstrual bleeding. Birth control pills may also resolve PCOS because they supply regular and consistent amounts of both estrogen and progesterone and thereby regulate monthly periods
References
- American College of Obstetricians and Gynecologists. Gynecological Problems: Polycystic Ovary Syndrome. 2007. www.acog.org/publications/patient_education.pdf/bp121.cfm.
- American Society for Reproductive Medicine. Patient’s Fact Sheet: Polycystic Ovary Syndrome. 2005. www.asrm.org/Patients/FactSheets/PCOS.pdf.
- Parker WH. A Gynecologist’s Second Opinion. (c) 2003; A Plume Book; Published by the Penguin Group, New York, NY.